A third wave of COVID-19 infections more brutal than the first two that came before is seriously ravaging some sub-Saharan Africa countries, most of them in southern Africa as the continent falls way behind the rest of the world in vaccinations.
The current rate of infections being experienced in sub-Saharan Africa is the fastest in the world so far. It has been reported that the latest (delta) variant is 60 percent more transmissible than earlier variants. In some countries, infections are already more than double, or even triple, their January/February peaks. For example, according to the South African health ministry, in South Africa alone, recorded infections have spiked from 800 per day as of April to more than 13, 000 per day in June. In Zambia, by mid-June, recorded infections were double the January second wave peak.
The first wave spared sub-Saharan Africa. The region did not experience infection rates seen elsewhere around the world. Six months later, sub-Saharan Africa experienced a second wave that spread faster than the first.
In a number of countries however, the second wave already pushed strained local health systems to the breaking point. Another six months on, the third wave has hit even harder with devastating effects. Health systems are teetering on the brink of collapse; hospital beds and oxygen supplies are dwindling as 14 countries report their worst levels of infection since the pandemic began. Governments in sub-Saharan Africa are facing serious difficulties in heading off an imminent crisis. In Zambia and Namibia, new cases have outpaced the January levels in a matter of only three weeks. Countries north of southern Africa need to build some level of resistance to stave off a new surge, otherwise it may already be too late.
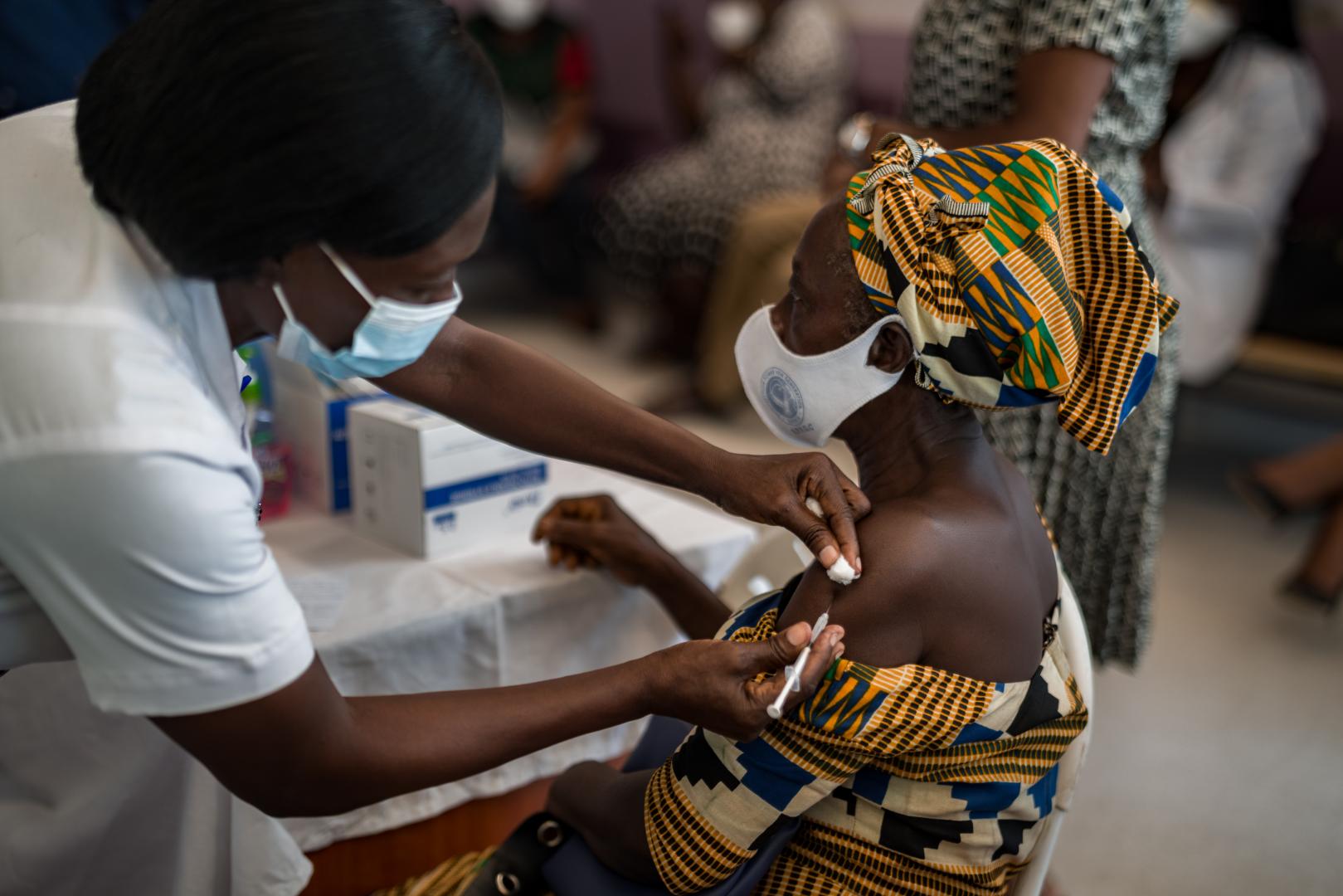
The only way to save the region from this vicious pandemic cycle is to swiftly implement a widespread vaccination program. At the moment, the vaccine rollout in sub-Saharan Africa is the slowest in the world. While in advanced economies an average 30 out of hundred adults are vaccinated, in sub-Saharan Africa, less than 1 percent of adults are fully vaccinated. This implies that even with limited supplies of protective equipment, most essential frontline workers continue to work without the protection of vaccination.
Africa Left Behind
Another fissure of global inequality has manifested. On one side of the chasm, Northern countries with good access to vaccines are slowly returning to normalcy with strong recoveries while on the other side of the chasm, sub-Saharan countries are left behind in panic as a new and deadlier variant of the disease overwhelms already strained healthcare systems. While lives are being lost in sub-Saharan, some of the world’s richer countries have stockpiled enough vaccines to cover their populations many times over.
What should be done?
Speed up the vaccine effort! Africa needs international assistance to save lives otherwise sub-Saharan Africa will see repeated waves of infection. If nothing is done, the new waves of infection will take an ever-increasing toll on lives. Even worse, they will wreak havoc on livelihoods of the region’s most vulnerable and paralyse economies.
Here are key steps we can take to ensure the needed vaccination targets are met:
- Deliver vaccines to sub-Saharan Africa soonest! Advanced economies that have bought up vaccines need to share their stockpiles. COVAX should be helped to turn received pledges of over half a billion doses into actual deliveries as soon as possible. COVAX and the African Vaccine Acquisition Task Team (AVATT), established by the African Union under the leadership of President Cyril Ramaphosa need to be fully financed to increase coverage of the African population.
- Vaccine manufacturers should speed up supply to Africa for the remaining part of the year. Advanced economies with vaccine manufacturing capabilities should encourage their manufacturers to speed up supply to Africa as demand in Northern countries begins to fall behind supply.
- Africa’s vaccination plans rely on two facilities, the Aspen facility in South Africa—a key supplier to AVATT— and the Serum Institute of India. Aspen must be made to be operational at full capacity and exports from the Serum Institute of India to COVAX should be resumed.
- Sub-Saharan African governments must be helped to build the capacity of public health systems to enable them to handle the current influx of cases. This involves the acquisition of vital COVID-19 health tools, including therapeutics, oxygen, and personal protective equipment must be accelerated now to help save lives.
- Finally, boost the region’s financing needs via a coordinated effort of the international community. Most sub-Saharan African countries do not have the fiscal space to finance the needed responses on their own. The region is already facing elevated debt levels and other pressing spending needs.
As has been noted before, the vaccination of Africa is not simply an African issue of saving local lives and livelihoods. It is also a global public good. If the Northern countries desire the most durable vaccine effort, the effort should cover everyone and every country.

Charlie Chilufya, SJ
Director of the Justice and Ecology at Jesuit Conference of Africa and Madagascar
Visit our campaign of “Equitable vaccine access for all”





